

By Yamam Almouradi, OD
Abstract
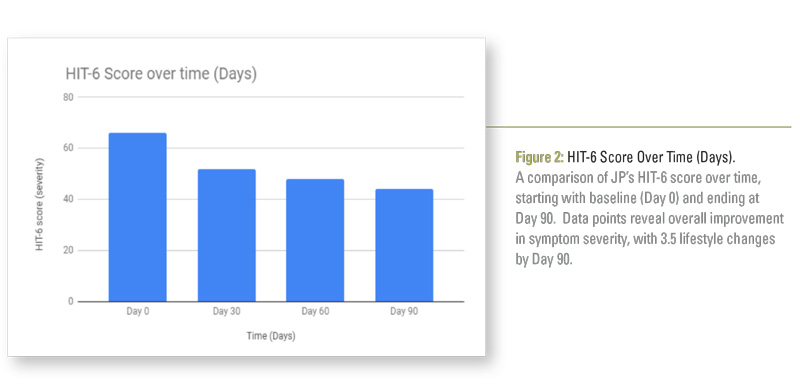
Ground-in prism and lens decentration are routinely utilized by optometrists and ophthalmologists to relieve symptoms of trigeminal dysphoria. This case study follows a symptomatic adult Caucasian male over 90 days to determine the effects of contoured prism technology on debilitating chronic daily headaches, using a validated Headache Impact Test (HIT-6). Qualitative data analysis reveals that full time wear of contoured prism lenses significantly improved patient HIT-6 score by 3.5 lifecycles. Most notably,
headaches that were frustrating and tiring enough to prevent activities of daily living on a highly frequent basis were completely alleviated by Day 90. Furthermore, there was notable subjective improvement of patient intake frequency of Advil and Excedrin, as the patient was able to decrease intake from “daily” to “on very rare occasion.” Additionally, the case study patient was able to discontinue Butalbital-Acetaminophen-caffeine 50 mg-325 mg-40 mg as well as Amitriptyline previously prescribed by his neurologist. Although a broader study is warranted, this case study suggests that adult patients suffering from chronic headaches significantly benefit from the addition of contoured progressive prism to their medical regimen.
Keywords: trigeminal dysphoria; contoured prism; chronic daily headaches; HIT-6.
Introduction
Historically, vision care professionals have utilized ground-in prism as well as lens decentration in their prescribed refractive error correction to relieve patients of various symptoms of Asthenopia1. Neurologically, the use of prisms or lens decentration to achieve a prismatic effect is derived from the over-stimulation of the fifth cranial nerve2, which has been linked in previous studies to trigeminal dysphoria3, among which chronic daily headaches (CDH)4 play a major role. In 2018, a randomized double blind quadruple arm study was carried out on 59 subjects to determine the effects of a treatment
using new technology contoured prism lenses on adult patients with symptomatic Digital Vision Syndrome. Chronic headache was a primary symptom in this 30 day study, which utilized a validated Chronic Vision Syndrome questionnaire (CVS-Q) for subjective assessment. This study included a single vision arm (18-45 year old patients) and a progressive arm (45+ year old patients). Results revealed that, on average, patients using contoured prism displayed 60% symptom reduction. Furthermore, 93% of subjects responded positively to the contoured prism treatment. Additionally, patients had a 30% increase in symptom relief when compared to usage of other premium lenses such as High Index lenses with blue light filters.
This case study investigates the efficacy of full time contoured prism wear on symptom frequency and severity of chronic headaches in adult patients. The author hypothesizes that if a positive correlation between full time contoured prism wear and decreased chronic headache symptoms is achieved, then prescribing contoured prism would provide an effective solution to improvement or complete resolution of chronic headaches not caused by systemic or ocular disease. Consequently, the author hopes to provide an effective prescribing or referral tool for optometrists and other health care professionals, respectively, for patients with chronic headaches.
Methods
One of the most symptomatic subjects in the Digital Vision Syndrome study was followed after the termination of the 30 day trial, for a total of 90 days, in order to determine the efficacy of full-time contoured prism use on chronic headache severity. JP is a 49 year old Caucasian male with a greater than 20 year history of severe chronic headaches that have interfered with his activities of daily living. He was prescribed several medications throughout these years in order to help him cope, as the intensity and high frequency of his headaches were preventing him from work, academia, and social activities. JP was instructed to complete a Headache Impact Test (HIT-6)5 , which is a tool that measures the impact headaches have on a person’s ability to accomplish his or her activities of daily living (Figure 1). HIT-6 was developed by an international team of headache experts from neurology and primary care medicine; it is a reliable and valid tool for discriminating symptom impact on chronic headache patients6. The scoring of HIT-6 assigns point values to symptom frequency, which increase proportional to symptom severity. A change of 6 points in a patient’s score over time is indicative of one lifestyle change. HIT-6 was chosen instead of MIDAS due to its higher accuracy in quantifying the intensity of pain rather than the frequency of headaches, the latter which is the main focus of MIDAS7 . In order to gain insight on headache frequency improvement over the 90 day trial, JP was asked to keep a daily log of his headache frequency, intensity, and usage of analgesic medications. He was consistent with his daily log and compliant with the full-time wear regiment of his lenses during the 90 day trial.


Results
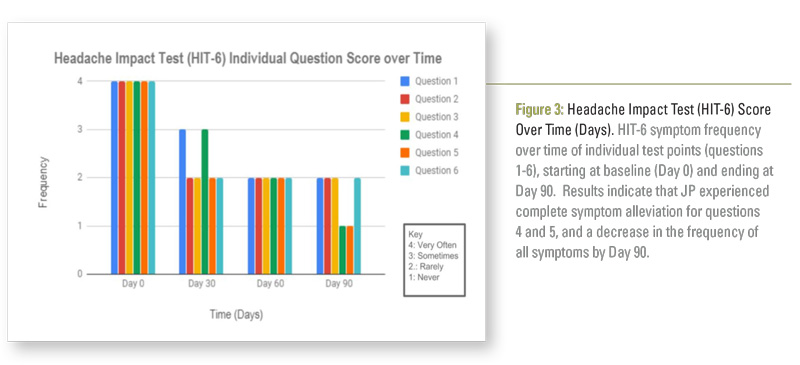
During baseline testing, JP’s HIT-6 score showed that he was experiencing disabling pain and symptoms that were interfering with his activities of daily living. His HIT-6 score improved steadily over the 90 day trial period, resulting in 3.5 lifestyle changes (Figure 2). Although all six specific headache symptoms in the HIT-6 questionnaire showed great improvement over time, questions four and five displayed complete symptom alleviation on Day 90.

Question four assessed patient headache severity leading to overall fatigue that prevented daily activities, and question five inquired about patient frustration or irritability secondary to headaches (Figure 3). By day 90, JP was successfully able to discontinue his two prescribed pain medications: Amitriptyline and Butalbital-Acetaminophen-Caffeine 50 mg-325 mg-40 mg; additionally, he was able to notably decrease his intake of Advil and Excedrin from a daily frequency to rare occasions.

Conclusion
As with any case study, some specific details might vary between patients, which in turn makes it difficult to generalize data points. However, the science behind prism use to alleviate symptoms of trigeminal dysphoria by over-stimulating the trigeminal nerve has been rigorously studied in previous years.
Contoured prism technology improves this technique by offering a customized prism that progresses down the lens to achieve increasing degrees of convergence relief as the patient shifts his or her focus from distance to a near target. This case study reveals that full time contour prism could in fact be used as a successful tool to alleviate debilitating headaches and notably decrease, if not abate, the need for daily pain medication in adults suffering from chronic headaches. The author recommends future studies to investigate contoured prism efficacy on chronic headaches and other trigeminal dysphoria symptoms
experienced by younger adult patients as well as children. Future larger scale studies are also warranted on adults with chronic headaches in order to achieve repeatable results.
References
1. Green, A. S. “The Value of Prisms in Eye Strain.” California state journal of medicine 10.11; 1912; 453.
2. Leigh RJ, Zee DS. The ocular motor periphery. In: Neurology of Eye Movements. 5th ed. Oxford University Press, 2015.
3. Thompson, Vance. “Binocular Vision: Keeping It Together.” Review of Ophthalmology, 5 Feb. 2019. www.reviewofophthalmology.com/article/binocular-vision-keeping-it-together [accessed 19, Feb. 2019.]
4. Ahmed, F., Parthasarathy, R., & Khalil, M. (2012). Chronic daily headaches. Annals of Indian Academy of Neurology, 15 (Suppl 1), S40–S50. https://dx.doi.org/10.4103%2F0972-2327.100002 [Accessed 15 Jan. 2019.]
5. Kosinski M, Bayliss MS, & Bjorner JB. A six-item short-form survey for measuring headache impact: the HIT-6. Qual Life Res 2003; 12: 963–974.
6. Yang, Min et al. “Validation of the Headache Impact Test (HIT-6™) Across Episodic and Chronic Migraine” Cephalalgia : an international journal of headache; vol. 31,3 (2011): 357-67.
7. Sauro KM, et al. (2019). HIT-6 and MIDAS as measures of headache disability in a headache referral population. PubMed-NCBI. https://www.ncbi.nlm.nih.gov/pubmed/19817883 [Accessed 20 Jan. 2019].



